A cataract is a clouding of the lens in the eye. When we see something, the light beams travel to our eye through the pupil and focus on the retina (a layer of light-sensitive cells at the back of the eye) thanks to the lens. The lens must be transparent in order to be able to focus the light properly on the retina. The opacity or cloudiness of the lens is called cataract.
Vision problems related with cataracts
If your vision has become blurred, cloudy or weak, or the things you see are not as bright or colorful as they used to be, a cataract may have developed in one or both eyes. Many people describe vision with cataracts as something similar to seeing through the dirty windshield of a car.
As a cataract slowly begins to develop, you may not notice any changes in your vision at first. But as the cataract progresses, you may begin to find that it interferes with your daily activities. Through a complete eye exam, your ophthalmologist (eye doctor) can tell you if the cataract or other problem causes your vision loss.
While cataracts are one of the most common causes of vision loss, especially as we age, they can be treated with cataract surgery. Since most cases of cataracts are part of the normal process of aging, they are not reversible. There are no medications or eye drops that can make the cataract disappear. Surgery is the only treatment.

The upper part of the lens is transparent. The bottom of the lens shows a cloudiness caused by cataracts.
If your lifestyle has not changed significantly, there may not be a need to remove the cataract. In some cases, a simple change of graduation of your glasses can help improve your vision. Contrary to popular belief, a cataract does not have to be “mature” to be removed. However, once cataracts are diagnosed, your ophthalmologist should regularly see if there are changes in your vision.
Cataract surgery for a clearer vision
When a cataract causes disturbing vision problems that interfere with your daily activities, your ophthalmologist may recommend surgery to remove the cataract. Through this surgery, the opaque natural lens is removed and replaced by an artificial implant called the intraocular lens or LIO.
You and your ophthalmologist can talk about the surgical procedure of cataracts, preparation and postoperative recovery, the benefits and possible complications of the surgery, in addition to the cost and other important information. By mutual agreement, you and your ophthalmologist can decide if cataract surgery is the right choice for you.
Symptoms of Cataracts
Most cataracts related to the progression of age, develop gradually. As a result, changes in the vision or signs of cataracts in their early stage of development may not be immediately perceived.
Little by little, as cataracts progress, you may experiment symptoms such as:
- Blurry or cloudy vision, painless;
- Difficulties to see at night or in situations with low light;
- Sensitivity to light and glow;
- Presence of halos around lights;
- Faded or yellowish colors;
- The need to use clearer light for reading and other activities;
- Frequent changes in the prescription of glasses or contact lenses; or
- Double vision in one eye
The only way to know for sure if you have cataracts is by doing a dilation exam, during which the pupil is dilated with eye drops. Your ophthalmologist may detect early signs of developing cataracts by looking at the lens of the eye.
Get an initial eye exam at age 40, when the first signs of illness and changes in vision may begin to appear. Your ophthalmologist (Eye Doctor) will let you know how often you should do follow-up exams. At any time, if you have symptoms or are at risk of developing the disease, consult your ophthalmologist. Since the risk of developing cataracts and other eye diseases increases with age, you should see your ophthalmologist annually from age 65 onwards. A complete eye examination will help rule out any other condition that may be causing blurred vision or other eye problems. Early detection and treatment of cataracts are critical to preserving eyesight.
Who Is At Risk Of Developing Cataracts?
Written by: Kierstan Boyd Reviewed by: Elena M Jimenez MD Mar. 13, 2014
Cataracts develop as part of the natural aging process, so eventually we are all at risk of developing them. By age 75, about 70 percent of people have cataracts. With age, little by little the lens of the eye becomes less flexible, less transparent and thicker. Subsequently, some areas of the lens become blurred as proteins begin to cluster in it.
Risk Factors for Developing Cataracts
The following factors increase your risk of developing cataracts:
- Advanced age;
- Diabetes;
- Family history of cataracts;
- Prolonged exposure to sunlight;
- Smoking;
- Obesity;
- Arterial hypertension;
- Previous injuries or inflammations in the eye;
- Previous ocular surgery;
- Prolonged use of steroids (especially the combination of inhaled steroids and oral steroids).
If you have any of these risk factors for developing cataracts, schedule an appointment with your eye doctor.
Cataracts Treatment
Written by: Kierstan Boyd Reviewed by: Elena M Jimenez MD Mar. 13, 2014
If your vision is just a bit blurry, a change in the prescription of your glasses may be all you need for some time. However, if after you change your eyeglasses graduation you still do not see enough to perform the activities you like or need to do, you should consider cataract surgery.
Through cataract surgery, the cloudy lens is removed and replaced with a clear artificial lens called the intraocular lens (LIO). Your ophthalmologist will discuss with you the surgical procedure of cataracts, the processes of preparation and recovery after surgery, its benefits and possible complications, as well as its costs and other important information.
Cataract surgery is often performed as an outpatient procedure and does not require hospitalization.
Cataract Surgery
Written by: Kierstan Boyd Reviewed by: Elena M Jimenez MD Mar. 13, 2014
Through cataract surgery, the cloudy lens is removed and replaced with a clear artificial lens called the intraocular lens (LIO). Often, cataract surgery is performed as an outpatient procedure and does not require hospitalization.
Preoperative tests for cataract surgery
Before surgery, the length of the eye is measured by a procedure called A-scan, and also the curvature of the cornea through a technique called keratometry. These measures help your ophthalmologist select the right lens implant for your eyes. Your eye doctor will also discuss with you the lens options available to you.
If you have previously had LASIK surgery or other laser surgery to correct vision, it is still possible to have cataract surgery. During the planning process for cataract surgery, provide your eye doctor your prescription for vision correction prior to LASIK surgery, if possible. This information will help your ophthalmologist calculate the correct LIO prescription. A previous refractive surgery may make it difficult to properly determine the right LIO; your vision prescription before that kind of surgery can help the surgeon correctly calculate the power of the LIO.
Cataract medications and surgery
If you have scheduled cataract surgery, be sure to tell your ophthalmologist all the medications and nutritional supplements you are taking. If you currently use drugs such as alpha blockers, or have previously used them for prostate problems, such as Flomax ®, Hytrin ®, Cadura ® or Uroxatral ®, tell your eye doctor. These medications can prevent the pupil from dilating properly during surgery, leading to possible complications. If the surgeon is aware that you have taken these drugs, he or she can adjust your surgical technique and adapt as needed, allowing the cataract removal procedure to be successful. Also tell your ophthalmologist about any other type of sedative you are using.
To reduce the risk of infection from surgery, your ophthalmologist may prescribe antibiotic drops to be used one or two days prior to surgery.
The cataract surgery procedure
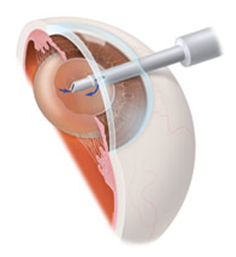
During phacoemulsification surgery, an ultrasound instrument breaks the center of the opaque lens and suctions it out.
The most common procedure used for cataract removal is called phacoemulsification.
After making a small incision at the edge of the cornea (the front of the eye), your ophthalmologist inserts a small instrument that uses high frequency ultrasound, which breaks the center of the opaque lens and carefully sucks it out.
After the opaque lens has been removed, the surgeon will replace it with an intraocular lens (LIO), an implant made of plastic, silicone or acrylic. The new transparent lens allows light to pass through the retina and focus properly. The LIO becomes a permanent part of the eye. In most cases, the LIO is placed on the iris, the colored part of the eye, and is called the posterior chamber lens. Sometimes, the intraocular lens should be placed in front of the iris. This lens is called anterior chamber lens. When the intraocular lens is in place, the surgeon closes the incision. Stitches may or may not be necessary. After the surgery, the eye doctor places a protective cover over your eye.
Recovery after cataract surgery
There will be a short period of rest time in the outpatient recovery area before you are discharged to go home. Make sure someone drives you home.
After your surgery, it is very important that you use the eye drops prescribed by your ophthalmologist to speed healing. You should also wear protective eyewear when sleeping, and special sunglasses for protection against bright light. Be sure not to rub your eye.
During the first week of recovery, you should avoid strenuous activities such as exercise or bending and lifting heavy objects (including anything weighing more than 25 pounds). You should also prevent water, dirt or dust from entering the eye, as these can lead to infections.
Your vision may be blurred for a few days or weeks after surgery. If you experience any pain or loss of vision, be sure to call your ophthalmologist.
Risks and complications of cataract surgery
Like any other surgical procedure, there are risks associated with cataract surgery. Risks and complications may include:
- Infection,
- Bleeding into the eye,
- Increased blood pressure inside the eye (glaucoma),
- Inflammation of the retina, and
- Loss of vision (partial or complete).


